|
10/7/2023 0 Comments Ekg pulseless electrical activityThere is no specific limit that defines hyperkalemia, but 5.5 mmol-1 is often referenced. It is commonly caused by impaired kidney functioning or excessive potassium release from cells. 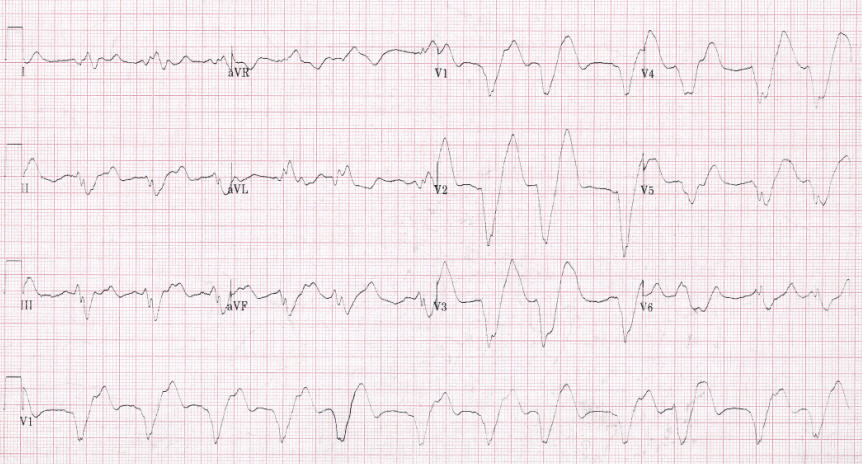
In addition, you may observe a widening QRS-wave. The first sign of hyperkalemia is typically taller & peaked T-waves. As such, it is crucial to the functioning of the heart, and either high levels (hyperkalemia) or low levels (hypokalemia) of potassium greatly increase the risk of cardiac arrest. Potassium is one of the key electrolytes that allows the body to contract muscles and conduct electrical signals through nerves. If the patient is suffering from metabolic acidosis, that can typically be resolved by administering sodium bicarbonate. If you determine they’re suffering from respiratory acidosis, that can be remedied by providing adequate ventilation. You can determine whether a patient is experiencing acidosis by performing an arterial blood gas evaluation. It can be either metabolic or respiratory, either of which can lead to cardiac arrest. Hydrogen Ion (Acidosis)Įxcessive hydrogen ions in the blood, otherwise known as respiratory acidosis, impairs the circulatory system, reducing oxygen uptake in the lungs. If needed, connect an oxygen source to supplement their normal respiration. If you observe your patient suffering from hypoxia, first ensure their airway is clear and their breathing is normal. This consideration can be a significant contributor to cardiac arrest. Respiratory depression, respiratory distress, slowing heart rate, or a pulse oximeter reading below 94% may indicate your patient is suffering from hypoxia. Hypoxia is a condition in which the body or a region of the body is deprived of adequate oxygen supply. Infusion of either standard saline or Ringer’s lactate should help to correct the issue. You may notice rapid heart rate and a narrow QRS wave on EKG, or significant blood loss, which would indicate hypovolemia may be a contributing factor. It can be a significant contributing factor to cardiac arrest. Hypovolemia is the decrease in the volume of blood in your body, which can be due to blood loss or loss of body fluids. In total there are twelve reversible conditions that make up the H’s & T’s: Hypovolemia When done close the diagram.These factors are primarily associated with PEA, but having a working knowledge of each will help you to diagnose the underlying cause of any ACLS-associated arrhythmia. View the cardiac arrest algorithm diagram. The pulse check should be performed simultaneously with the rhythm check when treating PEA since by definition PEA is an organized rhythm and could have a pulse that generates blood perfusion. 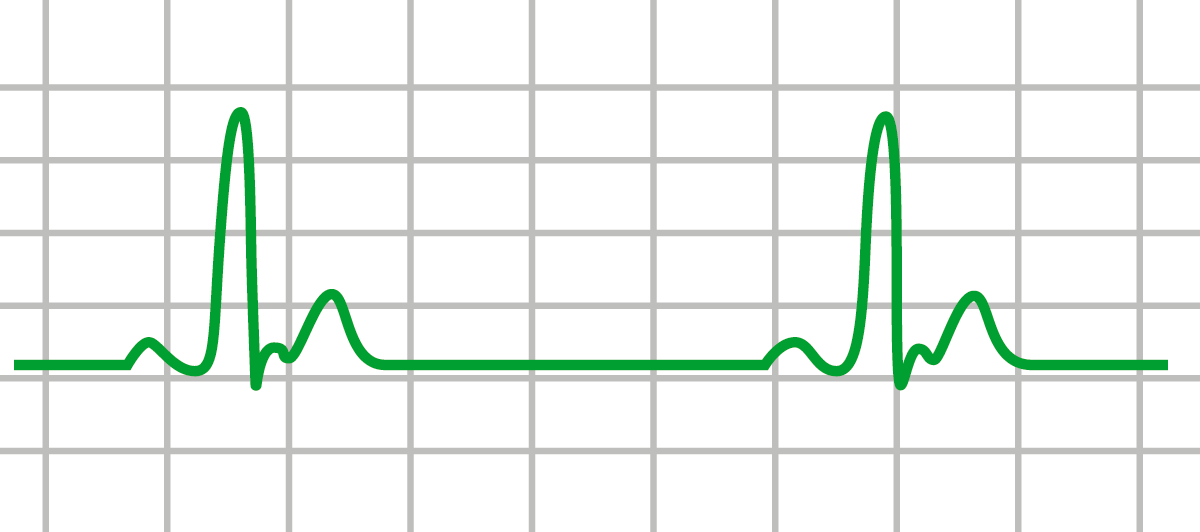
Limit the rhythm/pulse check to less than 10 seconds to minimize interruptions in CPR. 
High-quality CPR should be administered while giving epinephrine, and after the initial dose, epinephrine is given every 3-5 minutes.įor PEA a rhythm and pulse check should be performed after 5 cycles of CPR. When treating PEA, epinephrine can be given as soon as possible but its administration should not delay the initiation or continuation of CPR. Vasoconstriction is important during CPR because it will help increase blood flow to the brain and heart. The vasopressor that is used for the treatment within the right branch of the Cardiac Arrest Algorithm is epinephrine.Įpinephrine is primarily used for its vasoconstrictive effects. Medications used in PEA VasopressorsĪ vasopressor is a medication that produces vasoconstriction and a rise in blood pressure. Identification and correction of the cause of PEA. Positive outcome of an attempted resuscitation depends primarily on two actions: 1.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
